Balance your Estrobolome: Understanding the Gut-Hormone Connection
Post date: May 9, 2020
Author: Sarah Axtell, ND

Ever notice that when you are eating poorly that your PMS symptoms seem out of control? Do you experience “period poops”? Abdominal bloating or “PMS bloat”? You’ve heard about the gut-brain connection, but did you know that there is intimate connection between your gut and your hormones?
Recent research suggests that bacteria in our gut play a crucial role in regulation of hormones, notably estrogen metabolism. Meet the ESTROBOLOME (what a great word, right?!).
The Estrobolome is the “aggregate of enteric bacterial genes whose products are capable of metabolizing estrogen.”
Our ovaries produce estrogen. Estrogen is then sent to our uterus, breasts, and other organs to exert its magic (we need some estrogen…but it’s all about balance and metabolism of that estrogen). It’s then sent to the liver to become conjugated, or deactivated. Conjugated estrogens are then detoxed from the body after being converted to water-soluble compounds. These conjugated estrogen compounds are then sent to the kidneys and GI tract for excretion.
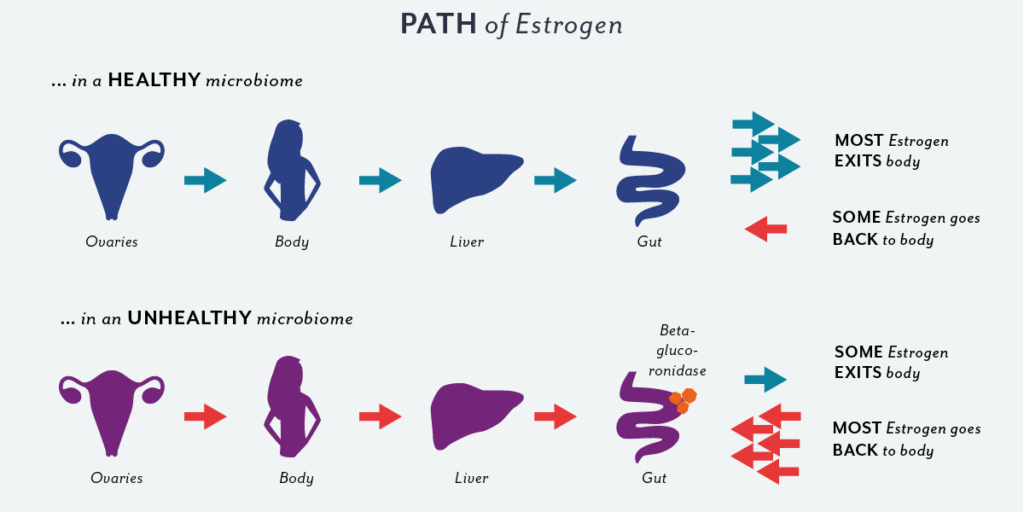
This is where the ESTROBOLOME comes in. When the conjugated estrogen compounds enter the gut, they can be deconjugated (activated) by certain bacteria species that have beta-glucoronidase activity. Too much beta-glucoronidase activity can lead to estrogen resorption into circulation…leading to estrogen dominant symptoms: weight gain, breast tenderness, abdominal bloating, PMS, cramps. In other words, gut dysbiosis (an imbalance of gut bacteria) can lead to poor elimination of estrogen, which can in turn lead to estrogen dominant symptoms (weight gain, heavy periods, fibroids, breast tenderness, abdominal bloating, PMS, cramps) and may even contribute to the development of obesity, metabolic syndrome, cancer, PCOS, fertility, and cardiovascular disease.
Summary:
In a healthy microbiome, most of the estrogen is excreted.
In an unhealthy microbiome, most of the estrogen is resorbed and sent back to the body, leading to estrogen dominant symptoms.
How to Improve Estrogen Metabolism by Supporting your Estrobolome:
DIET:
- Increase fiber. Good sources of fiber include pre-biotic foods that enrich the microbiome, such as artichoke, dandelion greens, chicory root, garlic, onion, leeks, and asparagus.
- Ground flaxseeds– 2 TBSP/day
- Eat fermented foods, such as kimchi, kombucha, plain yogurt, kefi, and sauerkraut,
- Eat 2 cups of cruciferous vegetables daily (broccoli, cauliflower, brussels sprouts, cabbage, bok choy).
- Reduce sugar.
- Reduce alcohol consumption. Excess alcohol consumption leads to higher beta-glucornidase activity and thus higher level of estrogen metabolites. This study showed that an altered microbiome due to alcohol consumption increases breast cancer risk.
Also, minimize antibiotic use when possible. This study revealed that antibiotic use can disrupt the intestinal microfloral metabolism of estrogens.
SUPPLEMENTS TO CONSIDER:
- DIM (cruciferous vegetable extract)
- Probiotics
- Calcium-d-Glucarate
Consult with your ND regarding which supplements and testing would be appropriate for you. The best test for hormone metabolism is the DUTCH test. To test for gut dysbiosis, we often do stool testing with our patients and breath tests (to rule out SIBO).
A happy gut= happy hormones= happy YOU!
Explore Related Posts:




